Contact Dermatitis Overview
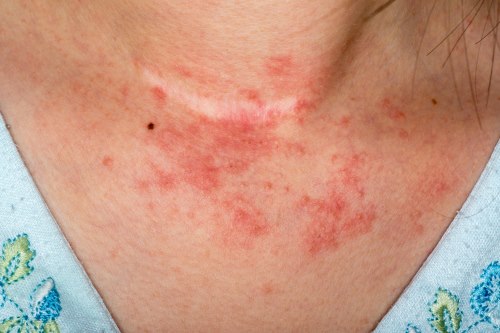
Contact dermatitis (CD) is a common skin problem occurring in 15% to 20% of people. It can have a significant financial burden with direct and indirect costs from lost time off work and school. CD may be allergic (ACD) or irritant (ICD). ICD is more common (80%) and can occur in anyone, especially after repeated exposure. Symptoms are a burning or stinging sensation with redness, swelling or peeling. Soaps, detergents, acids, bases, solvents, saliva, urine and stool are the most common triggers for ICD. Allergic CD, on the other hand, is seen in genetically predisposed and previously sensitized individuals who react to even low concentrations of the agent. Cosmetics, medicines, clothes dyes, as well as foods, rubber and poison ivy are common causes of ACD. Any topical cream or ointment may contain chemicals that irritate the skin. It is important to bring your personal products with you when you see your doctor so they can be examined as a potential cause of the dermatitis.
Contact Dermatitis Symptoms & Diagnosis
ACD presents with rash and itch. Acute reactions from poison ivy, sumac or oak are different from chronic lesions. Acute CD may look red and swollen with small fluid filled bumps (vesicles). Symptoms occur within a few hours of exposure. With chronic exposure the rash appears like “eczema” and the skin may thicken, scale or crack from scratching. The location of the rash depends on the allergen exposure. For instance, the rash associated with nickel allergy is located in areas of contact (underneath the belly button, ear lobes from earrings, around the neck from necklace). The rash from cosmetics is located on the face and particularly the eyelids. Patients with allergies to rubber gloves will present with hand dermatitis. Your allergist / immunologist can help differentiate ACD from other types of dermatitis including atopic dermatitis, psoriasis, seborrheic dermatitis and pityriasis rosea.
The diagnosis is made from history (what your doctor learns from talking to you including your hobbies, your work exposures, cosmetic/fragrance/hair dye/nail polish exposures, exposure to jewelry and other metals), physical exam and testing.
The patch test is used for the diagnosis of contact dermatitis. A small amount of diluted test allergens are applied to the skin under a patch of paper tape. The patches are placed on the back and are removed after 48 hours. Skin reactions are looked at and scored at a 48 hour visit and then again after 72 to 96 hours. Testing allows identification of chemicals you are allergic to so that they can be avoided in the future.
Contact Dermatitis Treatment & Management
Identifying the trigger is essential for correct advice to be given. Avoidance is key to treating the rash. If avoidance is not possible, the rash may become chronic, disabling and lead to a major impairment in quality of life. Advice might include:
• For acute symptoms, cold compresses can help with the itch.
• For patients with oozing lesions, Burrow’s solution (aluminum triacetate), calamine, and/or oatmeal baths can also be utilized.
• In hand dermatitis, avoiding excessive hand washing and using non-irritating moisturizers is recommended. Choose mild soaps, moisturizers, and detergents without dyes or perfumes. Wear gloves to protect your hands and other body parts from exposure if contact with these chemicals is unavoidable, however be aware that you can become allergic to chemicals in the gloves as well.
• In foot dermatitis, the use of barrier socks may be helpful.
• Wash skin immediately after contact with an allergen to limit the spread and severity of the reaction such as after known contact with a plant allergen (poison ivy).
• Apply covers over metal fasteners in clothing to avoid contact with nickel.
Topical Steroids
Topical steroids are anti-inflammatory medications. They help to get the rash under control more quickly and are usually applied 1-2 times a day. Topical steroids come in different formulations and strengths. Milder topical steroids such as hydrocortisone can be purchased over the counter. If the rash is not improving after 7 days or getting worse, you should consult your physician. A more potent topical steroid may be required, but should be used sparingly in sensitive areas such as the face, underarms and groin as they can thin the skin and cause stretch marks.
Antihistamines
Antihistamines may be given for the relief of the itch associated with CD but topical steroids are likely to be more effective in rash resolution. Sedating oral antihistamines promote sleep but may have side-effects including dryness, difficulty urinating, dizziness and impaired coordination. Sedating antihistamines should be used cautiously in elderly patients for all the above reasons and due to a potential association with dementia. These medications should be used in conjunction with consultation with your allergist / immunologist.
Topical Immunomodulators
Topical calcineurin inhibitors (pimecrolimus, tacrolimus) are anti-inflammatory agents that may provide another option in patients with ACD or ICD. However, they are not FDA approved for CD. They do not cause skin thinning, which is beneficial for the treatment of patients with facial dermatitis and dermatitis in other sensitive areas (bending areas, genitals). The most common adverse effects encountered are burning and itch at the application site.
Topical Antibiotics
These creams or ointments are sometimes used if there are open fissures and evidence of a secondary bacterial infection. However over-the-counter topical antibiotics are frequent causes of CD and should be used under the recommendation of your allergist / immunologist.
Systemic Steroids
These medications can be given by mouth or injection and may be needed if the rash is severe, associated with swelling, or if the rash covers much of your body. They will lead to rapid improvement and are usually considered safe when prescribed for short periods of time. However, systemic steroids can have significant side effects requiring close monitoring by your physician and are not recommended for long term therapy of CD. Some of these side effects can include weight gain, bone thinning, cataracts, glaucoma, easy bruising and sleep disturbances. It is also important to take these medications exactly as directed to avoid a flare in your dermatitis with rapid discontinuation as well as other side effects. Other oral medications that can be tried in difficult to treat cases include cyclosporine, methotrexate, azathioprine, and mycophenolate mofetil.
Phototherapy
Your allergist / immunologist may refer you to a dermatologist for light therapy if the rash is not responding to the above therapy.
References
1. Kostner, et al. Allergic Contact Dermatitis. Immunol Allergy Clin N Am (2017).
2. Fonacier L, et al. Contact dermatitis: a practice parameter-update 2015. J Allergy Clin Immunol Pract. (2015).
3. Fonacier L, et al. Current Strategies in Treating Severe Contact Dermatitis in Pediatric Patients. Current Allergy & Asthma Reports. (2012).
4. Boguniewicz M, et al. Atopic Dermatitis & Contact Dermatitis. Manual of Allergy & Immunology 5th edition. Editors: Daniel Adelman, MD, Thomas Casale, MD & Jonathan Corren, MD. Publisher: Lippincott Williams & Wilkins, Philadelphia, 2012, pages 215-242.
Find out more about skin allergies.
The AAAAI's Find an Allergist / Immunologist service is a trusted resource to help you find a specialist close to home.
12/11/2023