Eczema (Atopic Dermatitis) Overview
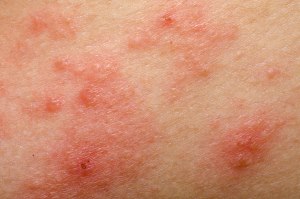 Eczema, also called atopic dermatitis, is a common chronic skin disease that usually starts in early childhood. One of the main symptoms of this condition is very itchy and dry skin. The skin becomes inflamed, red, irritated and scaly. Chronic inflammation below the surface of the skin is a major reason eczema occurs. Another reason this condition can occur is due to a variation in a gene for a protein called filaggrin. The alteration in this gene leads to a “leaky” skin barrier allowing excess water loss from the skin and occurs in up to a third of people of Northern European or Eastern Asian descent.
Eczema, also called atopic dermatitis, is a common chronic skin disease that usually starts in early childhood. One of the main symptoms of this condition is very itchy and dry skin. The skin becomes inflamed, red, irritated and scaly. Chronic inflammation below the surface of the skin is a major reason eczema occurs. Another reason this condition can occur is due to a variation in a gene for a protein called filaggrin. The alteration in this gene leads to a “leaky” skin barrier allowing excess water loss from the skin and occurs in up to a third of people of Northern European or Eastern Asian descent.
How the disease manifests can vary by age and race/ethnicity. In people with darker skin pigmentation, redness is often not appreciated; lesions may appear more violet colored. Eczema can occur on the face, arms, legs, hands, and feet. About half of those with eczema also have allergic conditions such as allergic rhinitis (hay fever), asthma, or food allergies. If the skin inflammation is not well controlled then infections due to bacteria, viruses, or yeast can occur.
Exposure to soaps, detergents, house dust mites, pollens, animal dander and some bacteria which contain “proteases” can all flare eczema. Proteases can further weaken the skin’s ability to retain water.
Moisturizers are used to improve the skin barrier. They act to help the skin retain moisture. Many people need to try several different moisturizers before finding the one which best suits them. Talking with your allergist is a great starting point. When there is active eczema, medicated creams and ointments that dampen down the inflammation are often prescribed.
Soft, non-irritating clothing that covers the arms and legs can help protect the skin from irritation.
Eczema Symptoms and Diagnosis
In infants and children, the rash often occurs on the scalp, knees, elbows, and cheeks. In adults the rash can occur on the creases of wrists, elbows, knees, ankles, face, and neck. The rash is usually itchy, red, and scaly in people with fair skin. Black or African American people more commonly present with extensor surfaces like knees and elbows. Scratch marks often occur due to the itchy nature of the rash. If one has the rash for a long period of time the affected skin can become thicker.
Dry skin can worsen the itching and rash starting what is described as an “itch-scratch cycle”. Rubbing and scratching the skin causes more irritation and thus more itching.
Infections can occur if the inflammation and itching are not well controlled.
It is important to talk with an allergist / immunologist about your rash. Other types of skin conditions such as psoriasis and contact dermatitis can look like an eczema rash. A common example of contact dermatitis is poison ivy. In addition, people with certain immune system problems and vitamin deficiencies can have a similar rash.
The ultimate diagnosis of eczema should be made by your allergist / immunologist.
Eczema Treatment and Management
The major goals of treatment are to improve quality of life and to minimize skin inflammation. Those with eczema should be able to participate in school, work, social, and family activities. Patients should feel healthy and satisfied with the skin’s appearance. Optimizing treatment to minimize social stigma is important. Your personal preferences should be taken into consideration when discussing treatment strategies.
Goals of treatment include improving the appearance of the skin, minimizing side effects of medication and improving sleep duration and quality.
Atopic Dermatitis Personalized Management Plan
Avoidance of Possible Triggers
Irritants: such as chemicals, soaps, detergents, fragrances, certain fabrics and smoke can further irritate the skin in those with eczema.
Some steps to reduce irritant exposure include:
• Wear comfortable clothing
• Wash all new clothes prior to wearing
• Keep fingernails short and smooth to prevent additional skin damage form scratching
• Use skin care products without fragrances
Environmental Allergens: Dust mites have proteases which can flare eczema. If one is allergic to animal dander this may have an impact on eczema as well.
Foods: The relationship between atopic dermatitis and food allergy is complicated. It is now understood that infants with atopic dermatitis may be more susceptible to allergen sensitization possibly through the defective skin barrier. It will be important to minimize skin inflammation and is not recommended to allergy test to a variety of foods without a history of reaction to that food or related foods. It is NOT recommended to avoid foods without a careful discussion with your allergist.
Stress: Stress and illness are other potential triggers.
Temperature: Heat, cold, or dryness can be potential triggers.
Contact Allergens: If eczema is difficult to control or there is a worsening after application of certain creams, lotions, soaps or shampoos, it may be worth exploring if you are allergic to an ingredient in these products.
Treatment of Atopic Dermatitis
Treatment options for atopic dermatitis have greatly expanded.
Topical Therapies: Topical means anything applied directly to the skin. There are many topical therapies.
• Ointments- tend to have more oil than water and are usually more thick
• Creams- A mix of oil and water
• Solutions- A more liquid form and can feel watery
• Lotions- Thicker than a solution but not as think as an ointment or cream
Moisturizing the Skin: Dry skin tends to worsen the itching and rash, therefore moisturizing and hydrating your skin is an important component to eczema care. After soaking skin in a lukewarm bath or shower, gently pat the skin dry and immediately apply a moisturizer on slightly wet skin to “lock” in the water and thus, improve dryness. It is important to know that moisturizers are NOT steroids. Petrolatum is a moisturizer that helps to seal in water. Some over the counter preparations containing components called ceramides (a type of lipid or fat) can benefit some people as well. Ceramides are naturally present in the skin and may need to be replenished in eczematous skin.
Topical Steroids: Topical steroids are anti-inflammatory medications that are used on the areas of rash. These steroids are not the same as testosterone or estrogen. When used properly as advised by your physician, topical steroids are safe and effective. One topical steroid may be stronger (more potent) than another, and thus, may improve the rash more effectively than a weaker topical steroid. However, the stronger steroid also has potentially more side effects including thinning of the skin, and thus potent steroids should not be used on certain areas, such as the underarms, groin area, and face. Usually, topical steroids found over-the-counter are not as strong as prescription ones. Bring all topical medications (they come in various forms, including creams, lotions, and ointments) to your allergist / immunologist, so the provider can review them.
Steroid pills or steroid injections (shots) are much stronger than topical steroids and can therefore cause more severe side-effects (including weight gain and bone problems). They should not become part of a well-planned care plan for eczema.
Topical Calcineurin Inhibitors: Topical calcineurin inhibitors are non-steroidal topical anti-inflammatory medications. They are usually second-line agents used if steroids are unsuccessful or to give the skin a break from steroids. As they are not steroids, these medicines can be used on eyelid and other facial areas, as they do not normally thin the skin. As with any other medications, they may have other potential side effects, so one must discuss them with your allergy / immunology provider prior to use. Tacrolimus and pimecrolimus are two examples of calcineurin inhibitors and are effective nonsteroidal treatments. These agents target inflammation in a different way than topical steroids.
Topical Phosphodiesterase Inhibitors: These are additional topical non-steroidal anti-inflammatory medications. Crisaborole is approved for ages 3 months and up and it can be applied twice daily on the face and body. Roflumilast is approved for ages 6 years and up and is applied once daily. These medications do not thin the skin like topical steroids.
Topical JAK Pathway Inhibitor: Ruxolitinib is a topical inhibitor of another inflammatory pathway called the JAK pathway. This is another possible treatment for eczema not responding to topical steroids. It should not be used for more than 8 continuous weeks and should be used on less than 20% total body surface area in those age 12 years or above.
Topical Aryl Hydrocarbon Receptor Agents: Tapinarof is a cream that targets a molecule called the aryl hydrocarbon receptor. It is a non-steroidal agent approved in ages 2 and up and is applied once daily to the face and body.
Systemic Therapies: Systemic means either anything you have to ingest my mouth or an injection. Current approved systemic therapies include biologics and small molecules.
• Biologics: Human-made proteins that are intended to be very targeted to one specific part of the immune system. These are administered by injection because they are not well suited to be given orally. Biologic medications have been approved for a variety of conditions including asthma and eczema. One biologic agent, dupilumab, has been approved for the treatment of moderate to severe eczema for ages 6 months and above. The biologics tralokinumab, lebrikizumab and nemolizumab have been approved for ages 12 years and older. Your allergist / immunologist can discuss biological medications with you.
• Small Molecules: Synthetic drugs that inhibit activity of enzymes. These are administered orally. Two oral JAK inhibitors, upadaticinib and abrocitinib, are approved for eczema in people 12 years and older. An allergist / immunologist can discuss the benefits and risks of these medications.
• Other Immunosuppressive Medications: In some cases of severe atopic dermatitis, other immunosuppressive medications can also be considered. These medications are not specifically approved for eczema.
Management Options
Phototherapy: This is a form of light therapy more typically performed by dermatologists to treat severe diffuse eczema of the body or severe hand eczema. This therapy is reserved for adults and children who fail topical steroids and other available treatment options. Ultraviolet light is categorized by wavelength and is called UVA, UVB or UVC. Narrowband UVB refers to the light spectrum at 311-313 nm and is most tolerated for treatment with the least side effects. Side effects can include sunburn and premature skin aging. Phototherapy may be used in combination with other treatment options.
Wet-Wrap Therapy: Wet wrap therapy is usually used for people with difficult to manage eczema. In this therapy, the skin is soaked in warm water for about 15-20 minutes and then is patted dry. Topical medications (typically, steroids or other anti-inflammatory medications, as described above) are then placed on the “rash” areas of the skin. Then, a wet (damp, not dripping) dressing (either gauze or cotton clothing) is applied on top of the rash areas. This is followed by a dry wrap material, such as elastic bandage, pajamas, or socks, placed over the wet dressing. For patient comfort, a warm blanket may also be used. Wraps are used typically for 2-6 hours or can be used overnight. The use of wet wrap therapy is individualized and typically used for flares of disease.
Antihistamines: Oral, or pill, antihistamines do not reduce the itch associated with eczema, as it is not triggered by histamine. Sedative antihistamines are sometimes used to help encourage much needed sleep at night. However, there are potential side effects, including increased sleepiness, or sedation during the day, increased dryness, and difficulty urinating.
Therapies for Associated Infections: Skin can become infected and topical or oral treatments may be required.
Bathing Strategies Including Dilute Bleach Baths: Very dilute bleach baths (typically, one quarter to one half cup of bleach mixed with 40 gallons of water bath) once to twice weekly may help improve the rash and may decrease the need for antibiotics. This should only be implemented after discussion with your allergy provider.
Stress-Relieving Therapies: Stress reduction techniques, such as biofeedback and other techniques may be used to improve mood and decrease anxiety associated with eczema.
Vitamins: There has been a recent increase in studies associating vitamin D deficiency with eczema. If you have been diagnosed with vitamin D deficiency (low Vitamin D level) by your physician, Vitamin D supplements may be prescribed.
Probiotics: Despite a lot of media attention on probiotics, at present, there is no conclusive evidence showing that probiotic use improves or prevents eczema, and it is not currently recommended in routine eczema care.
Allergy Shots (Allergy Injections): Allergy shots (giving injections of small doses of what you are allergic to, such as dust mites, under the skin in the arms) are currently approved for the treatment of asthma and allergic rhinitis (hay fever). Allergy shots can help some patients with eczema. Allergy shots are not the same as steroid shots, or steroid injections. Your allergist / immunologist can discuss whether allergy shots are appropriate for your eczema.
Summary
Eczema is a manageable condition regardless of age. There are many treatment options available. It may require a combination of approaches to achieve the best results. With careful evaluation and follow up with an allergist/ immunologist, patients with eczema can have a very high quality of life and enjoy favorite activities. A personalized treatment plan can be developed to align with an individual’s preferences.
References
Ahn J, Grinich EE, Choi Y, Guttman-Yassky E, Simpson EL. Emerging Systemic Therapeutic Biologics and Small Molecules for Atopic Dermatitis: How to Decide Which Treatment is Right for Your Patients. J Allergy Clin Immunol Pract. 2021 April; 9(4):1449-60.
Appiah MM, et. al. Atopic Dermatitis – Review of Comorbidities and Therapeutics. Ann Allergy Asthma Immunol. 2022 August; 129(2):142-9.
Brar KK, Nicol NH, Boguniewicz M. Strategies for Successful Management of Severe Atopic Dermatitis. J Allergy Clin Immunol Pract. 2019 January; 7(1):1-16.
Elias PM. Optimizing Emollient Therapy for Skin Barrier Repair in Atopic Dermatitis. Ann Allergy Asthma Immunol. 2022 May; 128(5):505-11.
Leung DYM. Targeting the Skin in Atopic Dermatitis. Ann Allergy Asthma Immunol. 2022 May; 128(5):481-2.
Singh AM et. al. Atopic Dermatitis and Food Allergy: Best Practice and Knowledge Gaps – A Work Group Report from the AAAAI Allergic Skin Diseases Committee and Leadership Institute Project. J Allergy Clin Immunol Pract. 2022 March; 10(3):697-706
Find out more about skin allergies.
The AAAAI's Find an Allergist / Immunologist service is a trusted resource to help you find a specialist close to home.
10/1/2025